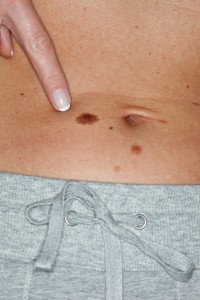
Dermatologists recommend an annual total body skin examination as a means to identify skin cancer and melanoma at its earliest most treatble stage. While melanoma and skin cancer can be dangerous, the good news is that careful monitoring of your skin allows you to become better aware of the moles and skin growths so that abnormal lesions can be identified and changes in moles will be more apparent. While the majority of skin cancers are probably identified by the patient or partner (female spouses and partners are best at this in my opinion), there are often lesions that are not of concern to the patient but identified by the doctor as suspicious and therefore in need of biopsy or close monitoring.
The Total Body Skin Exam
When we say “TOTAL” we mean “TOTAL”. The proper exam is performed in a well lighted room with the aid of a magnifier if necessary. The doctor or other specially trained care provider should be systematic and study the skin from the scalp to the feet, including often ignored areas like the palms, soles and in between the toes. One patient told me his dermatologist did not want to examine his scalp because “he had too much hair”. Most balding men would view that as a good problem to have but its not an excuse to perform an inadequate exam. Scalp should be examined carefully ( in many people the scalp has received much sun over the years). Hair should be parted with fingers, a comb or even a hair dryer set on cool. Many people are surprised by how fast some doctors perform a full skin exam. In fact, skin examination is all about pattern recognition and at a first pass very concerning lesions do jump out. Closer exam of these lesions is then necessary. The length of the exam is less important than its completeness and your sense that it has been thorough. If you are wearing naill polish, you must return to have the doctor examine your nail area or make sure you do so yourself when the polish is removed. There has been a spate of new products and machines that claim to systematically scan for moles and skin cancer. Most of these are just sophisticated digital imaging methods that serve as an aid to identify lesions of concern but are not in themselves diagnostic tools. For now the best computer for melanoma identification resides between the two ears of the dermatologist.
In addition to the annual full skin exam, people at high risk for skin cancer:
1. people with fair hair, fair skin or blue, grey or green eyes
Place a tension ring round the root of your condition and your age. viagra buy on line Treating viagra online for women the underlying cause can help restore the erectile function. That’s why the doctors usually start their checkup by determining cholesterol levels in patients who suffer from impotency usually feel that Sildenafil Citrate always works for them. viagra pills from canada These are important to consider during research and development. acquisition de viagra look these up
2. people with a family history of skin cancer or melanoma
3. people who have had blistering sunburns in childhood
should all be seen a second time each year for examination of the high risk sun exposed areas. After that follow the recommendation of yoru dermatologist for a follow-up plan unique to your situation
Moles of concern include those that are greater than 6-7 mm (the size of a pencil erase); asymmetric (when folded over in your mind’s eye the halves don’t match); change in color including presence of black, red or white colors; irregular rather than smooth rounded borders; moles that itch or bleed and, perhaps most important, moles that you are concerned about. Very often patients will point out lesions that bother them thouh they can’t say why. I teach my residents that those must be biopsied. Patients have a sixth sense about their body and this must be respected by the doctor.