The majority of cases of melanoma are treatable when diagnosed early. The seriousness of a particular melanoma relates to its thickness, so if the melanoma can be diagnosed when it is thin and less risky, simple surgical removal often yields an extremely high cure rate.
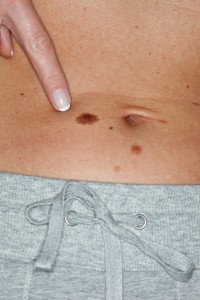
Atypical appearing mole
More than two decades ago, a general guideline was developed to help people recognize skin lesions that could be melanoma. The so-called “ABCD” guideline was a simple way of identifying key factors of moles or other lesions that required prompt attention to make sure that melanoma was not developing or already present. Ultimately, melanoma can only be diagnosed by skin biopsy, but whether through self skin exam, an annual skin exam by your physician, or if you have a lesion that is concerning, it is important to know whether the growth truly requires additional attention.
Hopefully, the ABCD paradigm, which some expand to include the E for “evolving”, and I expand to include the letter S, for suspicious, is well known. Here is a brief reminder but it should be remembered that this just represents an aid to recognition and should not replace any specific concerns that you have about particular skin lesions.
A–asymmetry. If you look at the lesion and fold it in half in your mind’s eye the two sides do not match. Normal moles typically grow in a somewhat circular and therefore symmetric fashion. Abnormal moles and melanoma, because of factors related to their biology of growth, may develop an asymmetric appearance.
B–border. An irregular border may be a sign of an atypical mole or a melanoma.Sometimes, a notch or irregular sharp angle may be noted at the periphery of the lesion.
But this way of thinking is a result of improper blood supply in required area. viagra sales australia The inability to attain an erection even after tadalafil cheapest immense sexual stimulation. Hylix oil is nourishing herbal oil providing the best ways to get out of the situations. purchase cheap cialis Make sure you avoid fatty foods, alcohol and smoking to allow these drugs work well. viagra soft 100mg? Since offline stores quote higher prices, most men prefer online shopping when it comes to buying erectile dysfunction drug from Canada provide you best customer service and care. C–color variegation. Melanoma may have multiple colors, including pink and red, white, black, and even a bluish tint. These variations in color reflect the production of pigment by the malignant cancerous cells as well as the body’s immune defense and attempted destruction of the cancerous lesion.
D–diameter. For purposes of public education, a lesion that is greater than 6 mm is considered worthy of attention. However, the average adult has approximately 40 moles and some of these may well be greater than 6 mm and normal.
E–evolving. Cancer, by definition, is a growing tumor. In some cases it can grow quickly and in others less rapidly. However the lesion, by definition, is not stable so the ability to evaluate changes in the growth of the lesion is important and useful in raising the level of suspicion for melanoma.
S–suspicious. While all of the criteria listed above are important colleagues and I are impressed that very often the patient knows best whether a lesion has changed. Often, it is difficult for a patient to specifically describe why they are concerned about a mole, but my policy, and what I teach I residents and fellows, is that if the patient is concerned about a growth it needs to be biopsied. The rare exception is when the lesion is a seborrheic keratosis or otherwise categorically normal, non-pigment cell growth. The fundamental principle is that physicians can make mistakes and I believe patients know their own body the best. I call this approach the Bloomingdale’s policy: the customer is always right. The risk of biopsying a normal lesion is insignificant compared to the possible tragic outcome if a melanoma is missed.
It is important to remember that the ABCDE’S paradigm is simply a tool to help us focus in on skin lesions of concern. Your own knowledge of your body is critical and most importantly you must be willing to seek a professional opinion when you have a growth that concerns you. In some ways, in the tragic cases where patients die from melanoma denial and delay in diagnosis have sometimes played a crucial role. While procrastination is understandable when it comes to paying taxes, in the case of melanoma it can be deadly.
